As a dad, you can’t take on the morning sickness burden once in a while… so, what can you do? Way more than you might think! Your support can help your partner throughout their pregnancy (and beyond). In fact, when fathers are involved during pregnancy, their partners tend to exercise more, attend more of their doctor’s appointments, and may even show improved mental health outcomes. But you have to know what’s going on.
In this article:
- First trimester
- Second trimester
- Third trimester
- Birth and postpartum
- Your wellbeing and mental health
So, whether you’re a seasoned dad just needing a refresher or a first-timer with no idea of what pregnancy entails, we’re here to help with a detailed week-by-week pregnancy for dads. For each trimester, we’ll discuss the changes happening to your baby and your partner, plus tips for what you can do as a dad to support your pregnant partner.
Editor’s Note: This pregnancy guide for dads was originally published in April 2021. It was updated in June 2024 with minor edits after being fact-checked again by Kristan Barczak who also happens to be a pregnant toddler mom.
First Trimester (Weeks 1 – 14)

Pregnancy for Dads 101: You’ve gotta learn how to count the duration. If you missed out on Greek and Latin roots in school, the prefix tri– means three. The most common way to break down the trimesters of pregnancy is through weeks and months. Generally speaking, a pregnancy lasts nine months and some change (technically closer to 10 months) with the first trimester being ~14 weeks, the second trimester being ~14 weeks, and the third being ~12 weeks. The first trimester starts on the first day of your partner’s last period and goes until the end of the thirteenth week. Within the first trimester, the baby and the mother change significantly. Let’s break it down.
Weeks 1 and 2
Technically, your partner isn’t pregnant yet. Medical professionals begin counting “weeks” of pregnancy from the first date of your partner’s last menstrual cycle, so “Week 1” is the week of your partner’s period (a little confusing, we know). But this is still an important couple of weeks if you’re trying for a baby. Sometime after your partner’s period ends, an ovum (egg) will be released into the fallopian tube, during a phase called ovulation.
You can use apps and methods like taking your basal body temperature to try to increase your chances of conception. For example, if your partner has a regular, 28-day cycle, every 28 days, they have their period. Then, approximately 14 days after their period begins, or 14 days into their cycle, they ovulate. Ultimately, this is the best time to try for a baby because your partner is fertile.
What Can You Do?
During this period, keep calm and keep trying for the baby. Also, make sure you’ve tackled a few things:
- Preconception checkup
- You may not be pregnant yet, but prenatal care begins long before fertilization occurs. A discussion with your gynecologist, together with your partner, is an excellent way to tackle any health issues. During the preconception checkup, your obstetrician-gynecologist (OB-GYN) asks questions about birth control, menstrual cycles, chronic conditions, medication, and diet.
At the end of the consultation, you and your partner find ways to boost fertility, increase the chances of pregnancy, and prepare a safe environment for fertilization to occur. It’s all about the information, and you should take in as much as you can.
- You may not be pregnant yet, but prenatal care begins long before fertilization occurs. A discussion with your gynecologist, together with your partner, is an excellent way to tackle any health issues. During the preconception checkup, your obstetrician-gynecologist (OB-GYN) asks questions about birth control, menstrual cycles, chronic conditions, medication, and diet.
- Take care of yourself and your partner
- Use this time to improve your physical, emotional, and mental health. At this point, you’re trying “to-be-a-dad-to-be,” but you also need to be a loving and supportive partner. Enjoy sex, cuddle, talk, enjoy healthy food, and go on dates. Of course, make sure you’re on the same page about your pregnancy and child to come.
- Insurance and Financial Planning
- If you’re trying for a baby, there’s a chance your insurance coverage isn’t top of your mind. Unfortunately, financial troubles are a quick way to strain through a pregnancy. We advise that you check on your insurance coverage before pregnancy.
Fortunately, most health insurance providers cover prenatal and maternity costs. If you’re a company employee, there’s a chance that your health insurance covers maternity costs. You can also research health insurance covers for your growing family at this point and plan for future out-of-pocket expenses.
Extend your financial planning to other expenses. Besides the prenatal care and insurance costs, you also have to care for a baby. Even if you don’t get down into all the details, it’s a great idea to have an amount in mind. You’ll likely find yourself exploring funds, insurance, savings plans, and business- and let’s be honest… some extra cash ain’t never hurt nobody.
- If you’re trying for a baby, there’s a chance your insurance coverage isn’t top of your mind. Unfortunately, financial troubles are a quick way to strain through a pregnancy. We advise that you check on your insurance coverage before pregnancy.
- Quit smoking and drinking
- This is a good time to stop unhealthy habits that might harm the baby. Your partner will need to quit smoking and drinking during pregnancy, and, as a partner, you should consider quitting smoking. Even second-hand smoke can harm a fetus.
Week 3
By the third week, your partner’s body is a flurry of activity. Remember the egg released during ovulation? It travels to a part called the fallopian tube. It sits and awaits fertilization. When sperm reaches the ovum and fertilizes it, a zygote forms.
Your partner also may not experience any noticeable physical or emotional changes just yet. However, the zygote quickly divides to form multiple cells. This multiplying cluster of cells is called a blastocyst, and it may be microscopic at this point, but it creates critical cells to form the embryo and the placenta. The blastocyst will start to slowly move towards your partner’s uterus, where it will begin to “implant.” Implantation typically occurs 6-12 days after ovulation, but it’s different for each pregnancy, and it could happen a bit sooner or later. If your partner implanted early, you might be able to get a positive on a pregnancy test during Week 3, but it could still be too early.
What Can You Do?
As the dad-to-be, make sure you continue to be supportive and caring. The wait for the positive pregnancy test can feel intense and emotional for your partner. Try to be understanding and find fun ways to take her mind off the wait.
Week 4
If you’ve gotten this far into the week-by-week pregnancy for dads, you’re already doing great. At this point, implantation has likely occurred and a hormone called hCG has begun to build—this is the hormone responsible for the positive on that test.
Even if your partner isn’t peeing on pregnancy tests at home, they may notice a missing period, which is a good reason to suspect pregnancy. Note: some people experience implantation bleeding. The bleeding usually occurs when the blastocyst burrows into the uterine wall. The bleeding is not severe and is significantly lighter than a period. It’s not a cause for alarm, but sometimes people mistake it for a period.
By the end of the fourth week, you might just have a pregnancy confirmed by an at-home test. Baby is tiny, about the size of a grain of sand.
Before we move on, a quick review of the hormones at play:
- Human Chorionic gonadotrophin (hCG) is a hormone that is produced 6 to 12 days after fertilization, which typically falls in Week 4 or 5. This hormone is formed in the placenta and increases as the pregnancy progresses. This is the hormone responsible for a positive sign on both a urine and blood test.
- Estrogen levels also increase. Usually, estrogen helps the body adjust for pregnancy. It affects development in the uterus, breasts, and cervix.
- Progesterone: The level of progesterone is usually higher than estrogen. It encourages implantation in the uterus and prevents contractions in the uterus that cause pregnancy loss.
Week 5
In this week, the hormones increase rapidly as the body prepares for the development of the baby. The earlier mentioned hCG rises quickly and sends a signal to the ovaries to stop releasing another egg for fertilization and instead release estrogen and progesterone to help with the baby’s growth. Due to a hormone shift, your partner misses their period (if they haven’t already).
You can also discover pregnancy in the fifth week of pregnancy (again, if you haven’t already). Once you get that positive, call your doctor. Some OBGYNs prefer to go ahead and bring your partner in to confirm the pregnancy around week 6. Others will have you wait until Weeks 8-10. If you need extra confirmation, women’s clinics will often provide free pregnancy tests in the meantime.
Inside the uterus, a baby, known as an embryo, is growing rapidly. The embryo divides into three layers and forms the foundation for the outer skin, the nervous systems, the inner eyes, and the ears. The middle cells give rise to the circulatory system, bone, ligaments, kidneys, and reproductive system. Lastly, we have the innermost layer, which develops into the lungs and intestines.
What Can You Do?
It may be a lot of science to remember, but don’t stress yourself into cramming every bit of it. What matters is that your baby is developing well. Once you confirm that you’re pregnant, there are several things you can do to make the pregnancy easier and safer.
- If you’re on laundry duty, wash it with unscented cleaners, especially if your partner complains about strong scents. Use unscented soaps, cut down on perfume, and avoid anything that triggers their nausea until the morning sickness goes away.
- Encourage your partner to consume meals high in iron, calcium, and vitamin C. You can also get them prenatal vitamins with guidance from your doctor. Prepare nutritious meals that provide adequate nourishment for your partner and the developing baby. Make sure you include a healthy amount of protein, carbohydrates, and vitamins in each meal.
- If your partner is experiencing nausea and vomiting, help them replenish their electrolytes by giving them liquids. Broths, diluted juices, and hot water with lemon can soothe them.
As soon as you and your partner suspect pregnancy, schedule a visit with your OB-GYN. Your prenatal appointments are crucial for your doctor to investigate your medical history (if they haven’t already done so) and deal with any health conditions that may affect your pregnancy’s health. If you have your first prenatal appointment during this week, you can expect the following questions:

- Your partner’s menstrual cycle, birth control, medical history, and past pregnancies (if any)
- You and your partner’s medical and family histories
- Medication used recently
- Lifestyle habits such as smoking, alcohol consumption, and substance abuse
- Travel details, especially to areas with malaria, Zika virus, tuberculosis, among other infectious diseases.
- The physician also checks your partner’s body weight, blood, pressure, and height. If they feel that your partner isn’t in tip-top shape for the pregnancy, they’ll make recommendations for you and your partner.
- The doctor also checks for vital issues such as the Rhesus factor, hemoglobin levels, and immunity and explores infections such as HIV and sexually transmitted infections that affect the baby’s health and development.
Your Baby’s Growth After Week 5
At this point, you will probably be aware that your partner is pregnant. Let’s quickly run through what your baby will go through in the first trimester, shall we?
Week 6
In the first eight weeks of the pregnancy, the baby is called an embryo. In the sixth week of development, the embryo begins to form a curved tadpole-like shape. It also develops the neural tube from which the spinal cord and the brain develop. Also, foundational structures for the eyes, ears, and arms grow. It’s also in this stage that the heart develops! Exciting!
Week 7
The embryo’s head and face grow significantly in the seventh week. The depressions that form the ears become visible, and the retinas start forming. New buds that eventually form the legs rise, and the buds forming the upper limbs develop into pads.
Week 8
In the eighth week of development, the lower limb buds grow into paddles while fingers form on the upper limbs. The head also undergoes significant changes. Shapes of the ears and eyes become prominent, and the upper lip begins to form. The neck also starts straightening out.
Week 9
In the ninth week, you can now call your baby a fetus. In this stage of growth, the baby forms elbows and toes. Their eyelids also become visible. You’ll also notice a larger head and better neck formation.
Week 10
Your embryo is officially a fetus! In the tenth week of growth, your baby’s head grows rounder, and the fingers and toes become less webbed and spread apart. Your baby can also bend their elbows at this point.
Week 11
By the eleventh week, your baby’s head grows broader, and the eyes separate. Other significant developments on the head include low-set ears and fused eyelids. The baby also grows buds that become future teeth. Inside the baby’s body, the red blood cells form the liver. At the end of the week, the baby’s genitalia also starts to grow.
Week 12
In week 12, the baby has intestines. Their facial features continue to develop, and they grow fingernails. Crazy, right?
Week 13
Up until this point, your baby’s head was the most significant part of the body. However, the rest of the body catches up. The kidneys and the urinary tract are functional, which allows the child to excrete amniotic fluid.
Week 14
The baby’s genitals develop, and their biological sex becomes more apparent. The baby’s spleen also begins to develop.
Meanwhile, What’s Happening to Your Partner in the First Trimester?
- As the baby develops, your partner experiences more physical pregnancy changes. First, the breasts become swollen, tender, and sore as they adapt to the hormonal changes.
- Nausea and vomiting become common as the body adjusts to the hormones. The best way to fight this is to eat in small portions, drink plenty of fluids, and consume fluids with ginger. It’s also best to avoid fatty foods and any foods that cause nausea.
- Your partner experiences more urination because the amount of blood increases. The kidneys work more frequently to clean blood.
- As hormone levels rise, your partner tends to experience more fatigue. Plenty of rest, nutritious goods, and exercise are helpful.
- Pregnancy hormones cause the relaxation of the valve between the stomach and esophagus, which causes heartburn. It’s crucial to avoid spicy meals, chocolate, and fried foods to prevent heartburn
- High levels of progesterone may cause slow movement of food, which causes constipation.
- Emotionally, your partner may experience mood swings. They may feel anxious, thrilled, and exhausted at the same time.
What Can You Do?

- Start your research!
- Now that your partner is approaching the second trimester, it’s time to start preparing for your new baby. We’ve got some great free checklists to get you pointed in the right direction, grab those right over here. Or, if you’re ready to jump in head first, consider an online course for expecting dads, we highlight 13 of the best ones out there here, and you can also check out Fathercraft’s own Father’s Ed—we’re biased, obviously, but we think it’s the most comprehensive and fun of the bunch.
- Let your partner get adequate sleep and rest. Take up more chores around the house and ask the rest of the family members to chip in. Also, drive your partner for doctor checkups as much as you can.
- Prepare healthy meals for the expectant mother. Include plenty of fluids and fiber in the diet to fight constipation. Try and avoid spicy, fried foods, citrus fruits, and chocolate to prevent heartburn.
- Help your partner prepare healthy meals they’re craving, and avoid those that cause nausea.
- Be supportive if your partner experiences mood swings you find challenging to understand. Talk to them, listen, and offer compassion.
- Visit the OBGYN with your partner to discuss the pregnancy and educate yourself on things dads should know about pregnancy. Remember to ask as many questions as you can about week by week pregnancy for dads to help you feel less anxious or uncertain about the baby on the way.
- Attend all first trimester tests and screening. The series of prenatal tests help determine the health of your baby. In the first trimester, your doctor may recommend testing your partner’s blood and performing ultrasounds.
First Trimester Prenatal Screening
Your doctor can check for genetic abnormalities before your child is fully developed. Some of the genetic disorders that can be detected include cystic fibrosis, hemophilia A, Down syndrome, sickle cell disease, and polycystic kidney disease. It’s best to consult your OB-GYN on possible congenital disabilities.
Your doctor will recommend ultrasounds (nuchal translucency) to check for:
- Increased fluid in the fetal neck
- Growth of the nasal bone. Sometimes, this bone is not detectable in babies with Down’s syndrome. If any of the results from the ultrasounds are concerning, your doctor will recommend you and your partner for genetic counseling.
- The due date
- Ectopic pregnancies
- The number of fetuses in the uterus
Your doctor may also order maternal blood tests in the first trimester to check pregnancy-associated plasma protein-A and human chorionic gonadotropin (HCG) levels. Abnormally high levels indicate a problem. The healthcare provider will also test the blood for the risk of carrying a baby with Down syndrome.
What Are The Risks In Early Pregnancy?
Unfortunately, while we all look forward to a great pregnancy, sometimes things do not go as expected. Early pregnancy loss or miscarriage sometimes occurs in the first trimester. Pregnancy loss mostly presents as cramping and bleeding. If you suspect you may be experiencing a miscarriage, you should call your doctor right away. Note: Some women experience light spotting in the first trimester as a normal pregnancy symptom. If your partner experiences spotting (i.e., light bleeding), you should still call your doctor (and they will likely tell you to go to the hospital), but it doesn’t necessarily mean you’re experiencing a miscarriage.
Miscarriage occurs in every 1 of 4 pregnancies, most often due to chromosomal abnormalities outside of you or your partner’s control. The risk is highest in the first 6 weeks before it steadily declines as you approach the second trimester. Miscarriage emotionally tough on both partners and physically tough on the pregnancy’s carrier. A few other notes on miscarriage:
- Lifestyle habits such as smoking and drinking also increase the risk of a miscarriage in the early pregnancy stages. It’s best to avoid smoking and drinking during pregnancy.
- Research indicates that the risk of a miscarriage increases with age. In this case, it’s crucial to stay in close communication with your OB-GYN.
- Even if your partner is bleeding and cramping, you can only confirm pregnancy loss with a checkup. Sometimes, the symptoms could be a sign of ectopic pregnancy. This is a condition where the implantation occurs in the fallopian tube instead of the uterus and is a medical emergency.
Second Trimester

Congratulations on reaching the second trimester of your pregnancy! The second trimester of pregnancy is between week 14 and week 28. If you’re already in this part of the pregnancy, you can smile a little because, in most cases, the risks of early pregnancy are sufficiently over. Check out our first pregnancy guide for men for more details.
Your Baby’s Growth in Weeks 15-27
The second trimester of baby development is intense, but even still, this trimester is often referred to as the “honeymoon phase” of pregnancy. By the end of this phase, the baby has functional internal systems, growing from around 3.5 inches and 1.5 ounces to 9 inches and 2 pounds. During the ultrasounds, you’ll see your tiny baby growing larger as they prepare to come to the world. At the same time, your partner’s nausea and fatigue are likely easing—but they aren’t experiencing the discomforts of late pregnancy just yet.
Week 15
The baby develops a scalp hair pattern. General bone development is intensifying at this point.
Week 16
The head becomes erect, and the baby starts moving its eyes. The ears also move to the correct position, and the skin thickens. You’ll also notice limb movement during ultrasounds.
Week 17
The baby’s activity increases, and they start rolling in the amniotic sac. They also develop toenails.
Week 18
Congratulations! Your baby can hear by now. The baby also faces forward and has a functional digestive system.
Week 19
In this week of growth, growth slows, and instead, the baby develops a protective coating called the vernix caseosa.
Week 20
At this point in the pregnancy, the baby sleeps and wakes. You may also feel the baby’s movements.
Week 21
Your baby has a fine layer of hair called lanugo which keeps the protective layer close to the skin. Your baby also develops the sucking reflex, which helps them suck on their thumb.
Week 22
In week 22, you can see the baby’s hair and eyebrows. Brown fat also begins to form in sites of heat production.
Week 23
The baby develops fingerprints, and the baby has rapid eye movement. Your baby can also hiccup at this point.
Week 24
Your baby’s skin begins to wrinkle and appears pink due to the blood capillaries on the skin.
Week 25
You baby can respond to your voice. However, the baby spends most of their time sleeping.
Week 26
The baby develops functional lungs.
Week 27
The baby’s nervous system and fat deposits continue to grow. This also marks the end of the second trimester.
Meanwhile, What’s Happening to Your Partner in the Second Trimester?
For most people, the second trimester is easier since the body adjusts to the changes. Nausea and fatigue decrease while more noticeable physical changes take shape. The baby bump also starts showing, and shopping for loose-fitting clothes becomes essential. Did someone say online shopping spree?
Your partner experiences the following changes:
- Body aches in the groin, back, and abdomen increase.
- Stretch marks begin to appear on the thighs, breasts, and stomach.
- A line running from the belly button to the pubic area might arise.

- Your partner may experience numbing or tingling in the hands—this is called carpal tunnel syndrome. Fortunately, you can consult your doctor for treatment.
- Patches of dark skin may develop on the face, lips, and cheeks—this is called melasma or pregnancy mask.
- The ankles, toes, fingers, and face may swell.
- Irregular, mild contractions in the abdomen may occur in the evenings, after physical exercise, or after sex. These are called “Braxton Hicks contractions,” and they’re just the body’s way of practicing. Unlike real labor contractions, these shouldn’t be painful and they don’t result in any changes to the cervix.
- Nasal congestion may occur due to swelling of the mucous membranes. Saline drops can help relieve nasal congestion, and applying petroleum jelly around the nostrils can help with dryness.
- As a result of poor circulation, your partner may experience dizziness from time to time.
- The gums may also become more sensitive. It’s best to brush teeth with a soft brush and be careful around the gums (the second trimester is the best time to see a dentist!).
- The risk of urinary tract infection (UTI) increases during pregnancy. It’s crucial for your partner to check for discomfort or pain during urination because it could indicate infection. Visiting the doctor is essential to treat UTI and prevent progression into the urinary tract and kidneys.
What Can You Do?
- Massage your partner’s back and pain points to help them with pain relief.
- Be reassuring and supportive of your partner’s physical changes.
- Help your partner consume more fluids or set up a humidifier for them to reduce nasal congestion.
- Maintain hygiene, especially in shared bathrooms, to reduce the risk of UTIs.
- Help your partner remain observant of the changes taking place. For instance, while weight gain and swelling are normal, sudden weight gain could indicate preeclampsia. If you and your partner are uncertain about something, schedule an appointment with your doctor.
- Attend doctor visits and second trimester testing with your partner.
- Do more research and read about pregnancy and newborn babies with your partner. We like The American Academy of Pediatrics’ Caring for Baby and Young Child, Birth to Age 5. And have we mentioned checklists can go a long way toward helping you feel prepared?
This is a great time to start preparing! Check out our newborn and baby essentials checklist here.
Second Trimester Doctor Visit Milestones
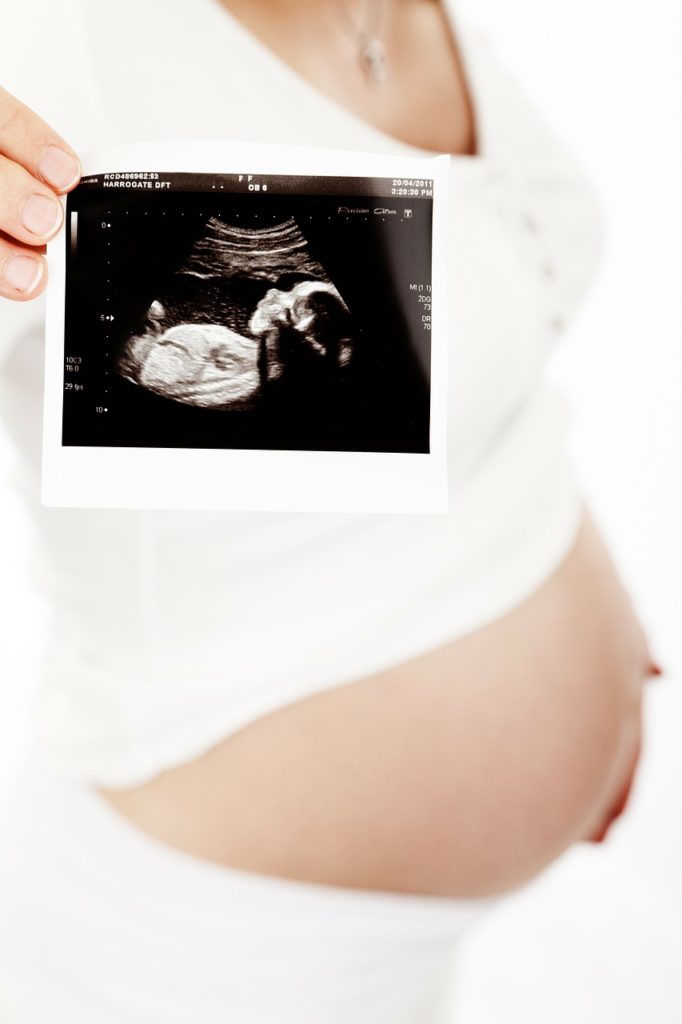
In the second trimester, you’ll continue to see your doctor every four weeks. They may recommend tests known as multiple blood markers, as well as a few other screenings:
- AFP screening checks for AFP levels in the blood. Abnormal levels may indicate abnormalities in the fetus’ abdominal walls, twins, Down’s syndrome, or spina bifida.
- Your doctor also checks for hormones such as hCG, estriol, and inhibin A in the placenta through blood tests.
- Your doctor may recommend amniocentesis between the 15th and 20th week of the pregnancy to confirm genetic defects and spina bifida. Typically, if blood work returns as “normal,” this won’t be recommended.
- You will receive an anatomy scan at 20 weeks. This is where you can find out the sex of the baby if you want! They also confirm that everything is forming as it should.
- Your partner will take a glucose test at around 26 weeks to check for gestational diabetes. The glucose drink makes some women feel sick and/or dizzy, so try to drive your partner if you can and plan to clear schedules for the rest of the day.
The end of the second trimester is a cause for celebration as you and your partner move into the third trimester. You can sing and talk to your baby because they can hear you and feel them as they move inside the uterus.
Third Trimester

Getting to the third trimester of a pregnancy is a relief for many parents. By this stage, the baby has grown considerably and may even survive in an incubator if born pre-term. Your partner may generally feel more tired as their belly grows bigger day by day. Fortunately, the end is in sight in the third trimester, and you can start counting down week-by-week pregnancy to the birth of your child or children. Let’s explore the baby’s development in the third trimester.
Your Baby’s Growth in Weeks 28-40
This is the final stage in your baby’s growth during pregnancy. You’ve made it all this way, watching as your partner nourished your baby from a cluster of cells to a moving, breathing being that you can proudly call your child. They don’t call it the miracle of life for nothing, folks.
Week 28
The baby measures around 10 inches and weighs approximately 2.25 pounds by the beginning of the third trimester. At this stage of development, the baby can open their eyes, and their eyelashes are grown. Their central nervous system is also in full swing as it regulates body temperature and breathing movements.
Week 29
As the baby continues to grow, motion becomes more common. Your partner can feel the baby grasp, stretch and kick.
Week 30
The red blood cells inside your baby are busy forming the bone marrow. At this stage, your baby can open its eyes. The head is also healthily developed by this week.
Week 31
The baby begins to gain weight rapidly. The majority of the significant development is already complete by this week.
Week 32
Remember the soft layered skin called lanugo that formed around your baby? It starts to fall off this week. At this point, your baby measures around 11 inches and weighs about 3.75 pounds. Your baby also starts practicing breathing in preparation for birth.
Week 33
Your baby’s pupils begin to detect light and change in size in response to the stimuli. The bones in the body also harden, although the skull remains soft.
Week 34
The fingernails reach maximum development this week. The baby also grows in size and measures around 12 inches and 4.5 pounds by this week.
Week 35
The baby’s skin smoothens, and the limbs grow in chubbiness. Gotta love the chubbiness.
Week 36
The baby is large at this point and consumes most of the space inside the amniotic sac. You’ll notice lots of movement on your partner’s belly as the baby stretches.
Week 37
By this point, your baby will likely have flipped head-down in preparation for delivery. At this stage, the baby weighs approximately 6.5 pounds.
Week 39
In the 39th week, the baby’s chest is prominent. In males, the testes descend towards the scrotum. The baby also gains fat to keep them warm.
Week 40
Your baby may have a length of 14 inches from their crown to rump and weigh around 7.5 pounds. It’s during this week that the due date arrives and you have to go to the hospital. However, remember due dates may vary, and your baby may come anywhere during this period.
Meanwhile, What’s Happening to Your Partner in the Third Trimester?

In the third trimester, your partner may generally feel more tired because the baby gains significant weight. It can be physically and emotionally challenging to get through this period. Here are some of the changes you can expect in the third trimester:
- Braxton Hicks contractions: Your partner may experience more of these mild contractions. Remember, these aren’t the real deal.
- Actual labor contractions: As you get closer to your due date, your partner may experience sporadic labor contractions. If they start to occur at regular intervals, don’t stop when changing positions or resting, or are accompanied by vaginal bleeding, call the hospital!
- Backaches: As the due date approaches, pregnancy hormones relax the connective tissue around the pelvic area in preparation for birth. Unfortunately, this causes discomfort and backaches. It’s best to wear comfortable flat shoes and avoid movement in this stage.
- Shortness of breath: Your partner may find themselves running out of breath frequently. Breathing exercises are recommended to keep the lungs strong.
- Heartburns: Pregnancy hormones tend to relax the valves between the stomach and the esophagus. This causes acid reflux, which is irritating.
- Prominent veins and hemorrhoids: Your partner may form spider veins along the face, neck, and arms. They may also develop painful varicose veins in their legs and get hemorrhoids in the rectal area. Soaking in warm tubs with witch-hazel helps with hemorrhoids.
- Increased urination: As the baby turns towards the pelvis, they place more pressure on the bladder, which causes frequent urination. Your partner may also have leaks when they sneeze, laugh or bend. Save the dad jokes for just a couple more weeks.
- The reality of birth, complications, and parenthood begins to set in: Your partner (and you) may be more anxious.
What Can You Do?
- As the pregnancy grows heavier and slightly uncomfortable, make your partner as physically comfortable as possible. Get them pillows and backrests to support their lower back. Support your partner in taking more naps… their body is doing a lot of work!
- Avoid highly acidic meals, fried foods, citrus fruits, and spicy food to prevent heartburn.
- Help your partner elevate their legs and frequently exercise to reduce swelling in the legs. Draw warm baths for them to soak in and relax.
- Talk to your partner about the baby, birth, and plans for the child’s future. Make sure you’re on the same page to reduce stress.
Pro tip: Read our full third trimester checklist here.
Prenatal Care
Once you enter the third trimester, your doctor or midwife will ask you to come in every two weeks until 36 weeks. Then, you’ll visit once a week until the baby makes their appearance. Your doctor will assess:
- Symptoms of discomfort
- Weight gain
- Blood pressure
- Risk of Preeclampsia: The doctor performs a urine test to find albumin, a protein that indicates preeclampsia.
- Risk of Hyperglycemia: The doctor checks the urine for glucose levels
- Baby’s heartbeat
- Baby’s position in the uterus
- Gestational diabetes: The doctor checks all symptoms that indicate the development of diabetes during pregnancy
- Group B strep: This bacteria develop in the vagina or rectum and may cause severe infection to the baby. The doctor recommends antibiotics if your partner has this bacteria.
- Anemia: during pregnancy, many people develop iron deficiency anemia. If your partner has anemia, they don’t have enough blood cells to circulate oxygen, making them tired.
- Your partner may also take an additional shot of vaccinations for diphtheria toxocoid and acellular pertuisis despite their vaccination status to prevent the unborn child from contracting whooping cough.
Birth: What To Expect

There are a few events that will trigger THE big trip to the hospital:
- Regular labor contractions occurring every 10-15 minutes apart for at least an hour and that grow in intensity
- Your partner suspects their water has broken (it’s not like the movies! Your partner’s water likely won’t break until after contractions have begun, and it’s usually not a whole “scene”—it can be a trickle)
- The day of your scheduled induction or c-section has arrived
More on labor and delivery below:
Labor
First, remember that labor is a natural process, which means it starts and proceeds at its own pace. Most of time, if labor begins naturally, it will start with mild contractions that build in intensity and become closer together.
It’s possible that your partner’s water could break before they feel contractions (although it doesn’t happen like the movies). Typically, this will feel like an uncontrollable trickle of water that doesn’t stop—this is the amniotic fluid leaving your partner’s body. No matter what, you should call the doctor if your partner’s water breaks. They’ll need to be monitored for infection. But if the color of the fluid is green or red, it becomes a bit more urgent. Sometimes, babies poop in the sac. It happens. But it can cause issues. So, just like the classic nursery rhyme: “If it’s yellowish, then we’re mellowish. If it’s red or green, GET YOUR ASS TO THE HOSPITAL!” Or something along those lines.
[Editor’s note: If this you, don’t fret! It actually happens a lot—it happened to me. I was already in the hospital, and I barely knew there was a problem. Our baby was born healthy. That said, it can be a medical emergency, and we are not medical professionals here at Fathercraft, so be sure to call.]
During labor, the contractions cause the cervix to open and soften. These actions allow the baby to move into the vaginal canal. In the early stages of labor, the contractions are irregular. Your partner may also notice pinkish discharge, usually because of the mucus from the cervix. The early labor may last for a few hours or days.
This period is uncomfortable, but until the contractions increase in frequency, you and your partner have to wait it out. You can encourage your partner by helping them:
- Take showers and baths
- Go for slow walks
- Change positions
- Have relaxing conversations or listen to calming music
- Practice breathing exercises
After early labor, active labor begins. In this stage, the contractions are frequent and intense. The cervix dilates by 3-4 inches. Your partner may also feel:
- Pressure in their back
- Nausea
- Leg cramps
- Pain
Active labor typically lasts up to eight hours, although it could go longer. As the pain increases, you can help your partner by:
- Helping them roll on a birthing ball
- Practicing breathing exercises
- Taking warm showers
- Providing gentle massages
- Changing positions
- Taking walks
The final stages of active labor are excruciating and uncomfortable for your partner. Contractions come in around 60-second intervals. They may also feel like delivering the baby at this point (this is called “transition,” and it typically means your partner is dilated 10cm).
Delivery
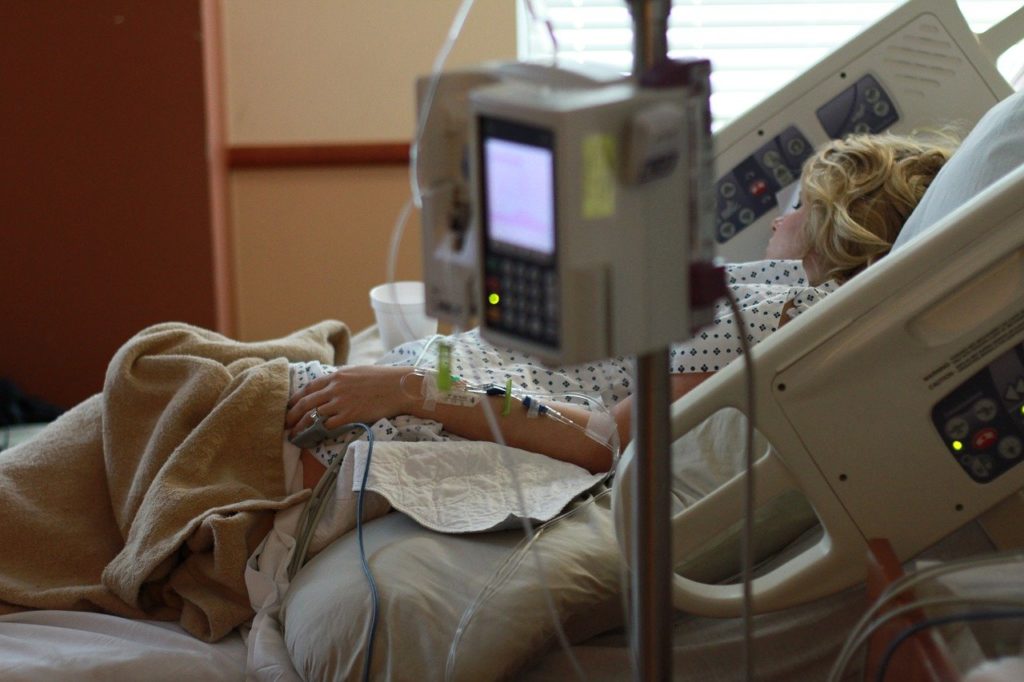
The birth of your baby could be a few minutes to several hours. It all varies depending on your partner and the baby. If you’re in the delivery room with your partner, the midwife or doctor will ask them to push the baby. It’s a challenging process, even with pain management, and one that requires lots of encouragement and motivation from you. Your partner can push the baby out while lying down, squatting, kneeling, or standing. You may find that your partner starts to doze off between contractions—this is normal and caused by hormones (and exhaustion).
Once the baby’s head is out, the rest of the body follows shortly. Sometimes, the doctor may recommend an episiotomy, a small cut on the perineum, to prevent injury during birth. The healthcare providers clear the airways and cut the umbilical cord as necessary. After the birth of the baby, the third part of labor and delivery begins. Your partner will experience mild contractions and birth the placenta.
The doctors may provide medication to minimize bleeding during the delivery process. After the placenta is out, contractions continue to return the uterus to its normal size. Your healthcare providers will also examine your partner to ensure that their body recovers. They’ll do something called a “fundal massage” to prevent hemorrhaging—it feels nothing like an actual massage and is actually pretty painful, so be prepared for more hand-squeezing. If stitches are necessary, the doctors will do them after the placenta is out.
Epidural
An epidural is a common method of pain relief. Many people request epidurals to help manage the pain that comes with labor. The epidural anesthesia relieves pain in a specific region without blocking total sensations. Before your due date, talk to your doctor or midwife about different epidural options.
Induced Labor
Labor induction is the use of interventions and medication (e.g., “pitocin” or synthetic oxytocin) to induce labor. There are several reasons why your doctor may induce labor:
- When the water has broken, but contractions have not started
- When it’s past the due date and contractions have not started
- When there isn’t enough amniotic fluid around your baby
- When the fetus stops growing at the expected rate
- When your partner has an infection in their uterus
- When the placenta separates from the uterus before delivery
- When your partner has medical conditions such as kidney disease, diabetes, or obesity
- Elective induction: You and your partner may choose to induce labor even when it’s not medically necessary. For this to happen, your baby should be at least 39 weeks old. This procedure may be available to people with rapid deliveries in the past and live far from health centers.
Are there risks of induced labor? As with most medical events, there are. Here are some of the risks you should know:
- Failed induction: The procedure may fail, which means that your partner may have to undergo a c-section to deliver the baby.
- Low heart rate: The medication used to induce labor causes rapid contractions that affect the baby’s heart rate and lower oxygen supply to the baby.
- Uterine rupture: if your partner has had a previous c-section or uterine surgery, inducing labor may cause rupturing.
- Bleeding: Induced labor increases the risk of severe bleeding after delivery.
- If your partner has had a c-section, undergone uterine surgery, or if the placenta is blocking the cervix, the doctor cannot induce labor.
- If the baby is lying sideways (traverse) or buttocks first (breech), your healthcare provider cannot induce labor.
In general, it’s helpful to know that many doctors considered induced labor to be a “high-risk” delivery, so your partner will need some extra monitoring. It’s always best to discuss the benefits and risks with your doctor or midwife when making a decision about induction.
C-Section
What if a vaginal birth does not happen? In some cases, your partner may have to deliver the baby through cesarian delivery or a c-section. This is a surgical procedure that takes the baby out from the abdomen or uterus. For first deliveries, a c-section may not be the obvious option until labor begins. However, if your partner has had a c-section before or develops complications with the pregnancy, your healthcare provider may plan for a c-section. There are several reasons why your doctor may recommend a c-section.
- If the labor stalls and the cervix fails to dilate
- If the baby is in an abnormal position. If the feet or buttocks are facing the cervix, the baby is in a breech position. If the baby is facing the cervix shoulder first, they’re in a transverse position.
- If your partner is carrying more than one baby
- If the placenta covers the opening of your cervix
- If a section of the umbilical cord comes out of the uterus before the baby
- If your partner has health conditions such as genital herpes or heart disease
- If your partner has pelvic fractures or fibroids covering the birth canal
What To Bring To Hospital
Sometime in the third trimester, you’ll want to pack the hospital bags. Here’s what we recommend including:
- Baby pajamas, swaddles, hats, socks, diapers, burp cloths, baby bottles, and pacifiers if you’re using them (the hospital will provide blankets, hats, diapers, and formula if needed, so try to use their things and save your own)—your partner might want to pack a “going home” outfit for baby
- A properly installed baby car seat you know how to use
- Loose clothes that are easy to throw on
- Comfortable house slippers for you and your partner
- Select a calming playlist or bring some essential oils for aromatherapy
- Hygiene products such as toothbrushes, toothpaste, pads, shower essentials, underwear, and deodorant
- Snacks and a water bottle
- Charging cords
- Pillows and blankets
- Books, laptops, or anything else your partner might want if they’re feeling mellow
- Pictures, affirmations, or anything else that might help your partner during labor
Note: The hospital will most likely provide anything your partner needs for postpartum care.
Postpartum
You’ve made it to the end of the pregnancy road, but your partner will still need your support while they heal from labor. The postpartum period is often thought of as the first six weeks after delivery, although research shows it can take up to two years for your partner to feel fully “themselves.”
During the postpartum period:
- Your partner may be trying to establish a breastfeeding relationship. You can help by attending appointments with lactation consultants, washing pump parts, and helping position your baby (also: warding off nosy visitors with unsolicited opinions).
- Your partner is healing from a vaginal birth or c-section.
- Vaginal birth: Healing period varies based on if there was a tear and its severity. Your partner may also be taking iron supplements to help with the loss of blood. Encourage them to rest as much as possible.
- C-section: Healing period may last longer than vaginal birth, as the incision scar heals. Your partner should exercise caution getting in and out of bed and moving up and down stairs. They may need help with everyday tasks for awhile.
- Your partner may exhibit signs of postpartum anxiety or depression. Research shows these signs can present anytime in the first year, up to the fourth year. Watch for signs and encourage her to speak with her doctor if she’s not feeling like herself.
- You and your partner will navigate any entirely new family dynamic—ask for help when needed, try to get rest, and remember you’re on the same team.
A note on your mental health
We like to keep things light around here, but you can’t be partner you want to be if you’re not feeling like yourself! You may not have carried the baby, but newborn life can still take a toll on your mental health. Research shows that 1 in 10 men exhibit signs of postpartum depression as well, due in part to change in hormones that you will actually experience, too. Watch out for these symptoms of paternal postpartum depression, and reach out if you need help:
- Anger/irritiability/violent outbursts
- Disconnection from partner and baby
- Loss of focus and interest in activities
- Physical symptoms like stomach and back aches
- Working a lot more or a lot less
- Thoughts of harming yourself or others
If you or your partner need help, call or text one of the following hotlines, or reach out to your doctor:
- Postpartum Support International (PSI): (800) 944-4773 (call or text)
- National Maternal Mental Health Hotline: (833) 852-6262 (call or text)
- Substance Abuse and Mental Health Services Administration (SAMHSA): (800) 662-4357 (call)
What’s next
Well, you made it! At least you made it to the end of this article. And you and your partner will make it through pregnancy too. And, educating yourself can go a long way toward helping you feel more prepared. That’s what we’re all about here at Fathercraft, learn more here.






